For the second time in two years, the so-called World Health Organization (WHO) has declared monkeypox, now rebranded as mpox, a public health emergency of international concern. As we shall see this is a rerun of covid-19 with somewhat poorer data this time round. But their confidence in their confidence game is quite remarkable. A quick two graph blast by Jessica Rose and another revelation by the ever-brilliant Dr. Peter McCullough will show their shenanigans to be a conspiracy to commit murder for profit on a global scale.
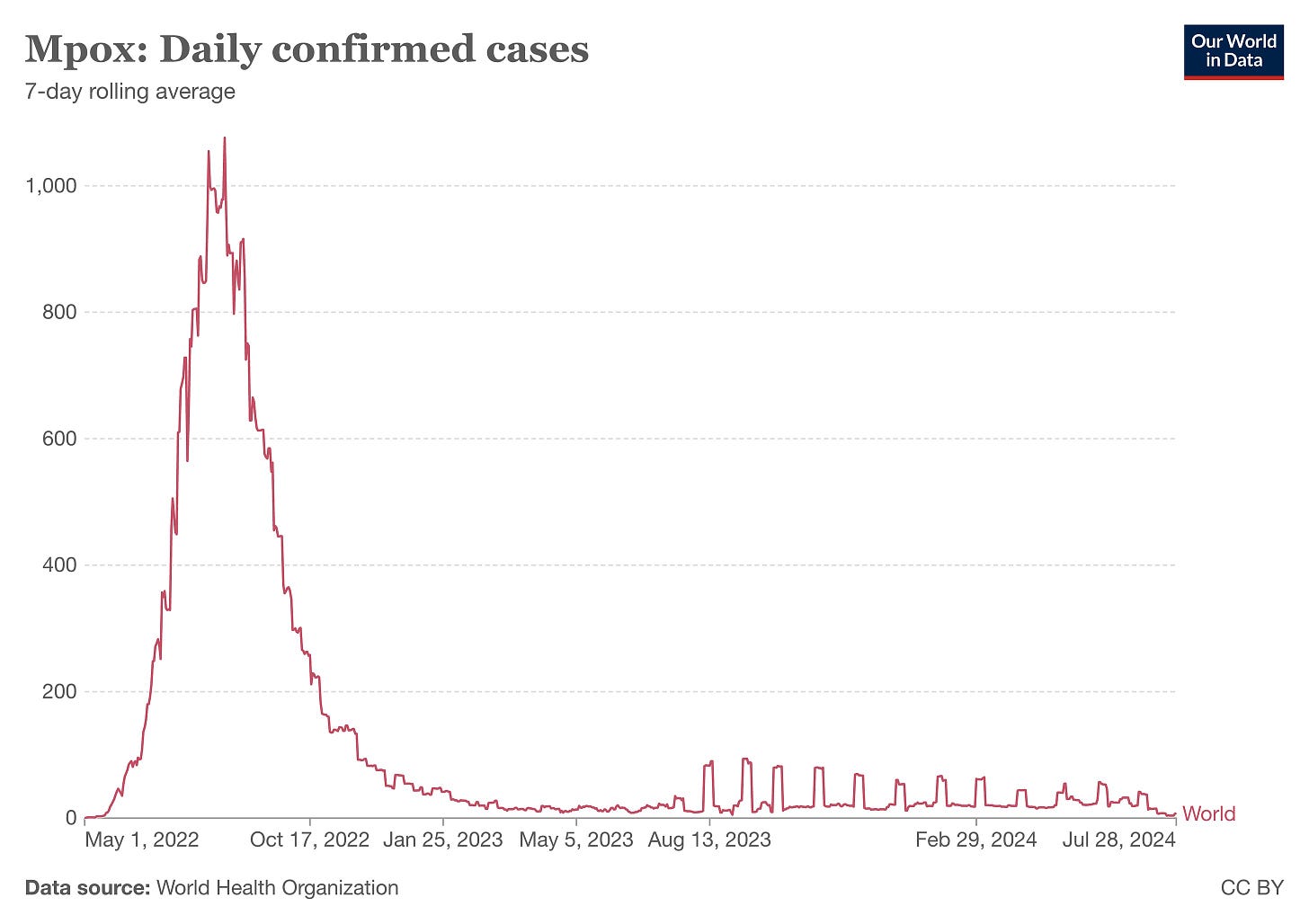
The number of (mpox) “Daily confirmed cases” worldwide according to Our World in Data.
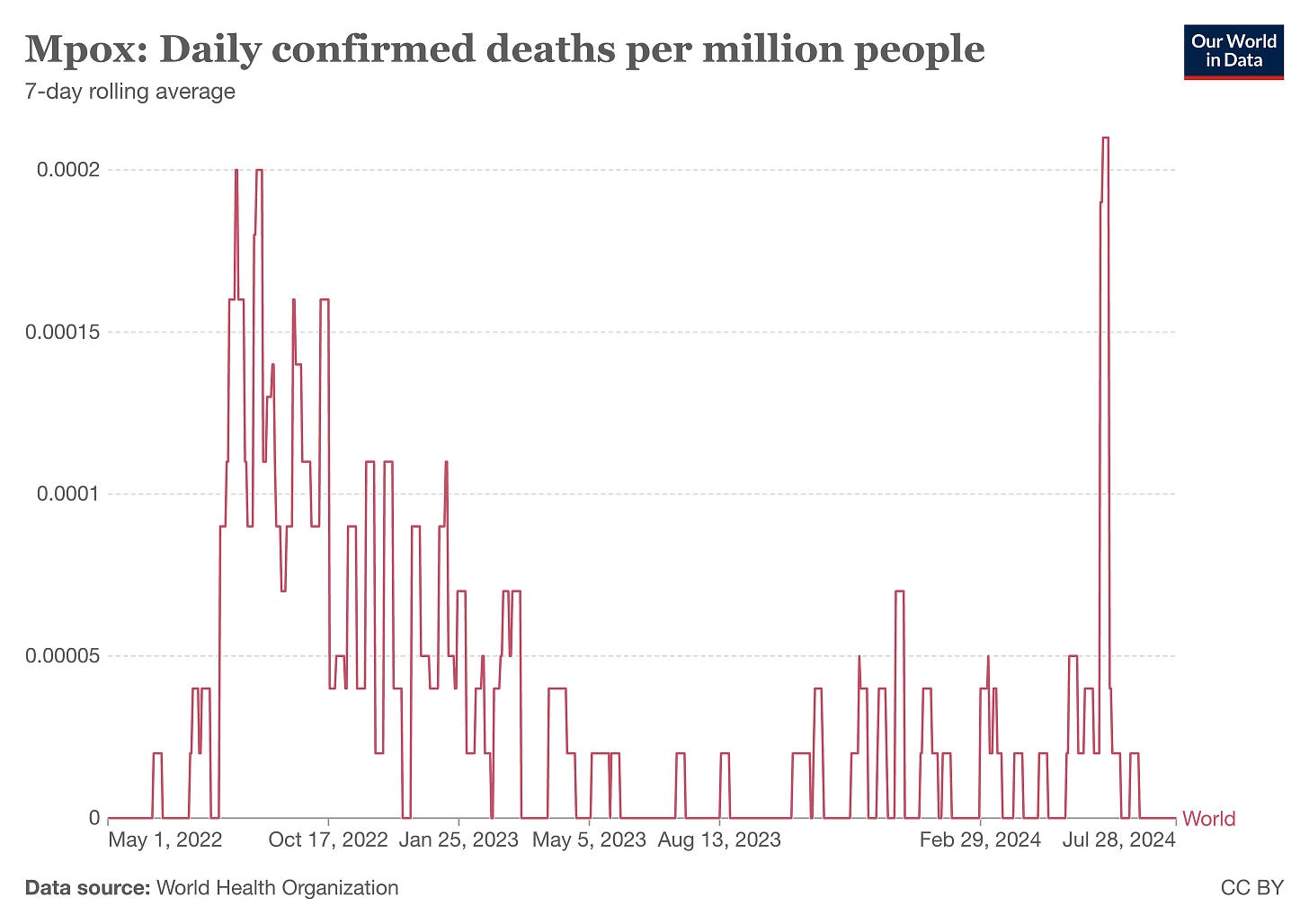
Then contextualize this with regard to “deaths”.
Source: Edouard Mathieu, Fiona Spooner, Saloni Dattani, Hannah Ritchie and Max Roser (2022) - “Mpox” Published online at OurWorldInData.org. Retrieved from: 'https://ourworldindata.org/mpox'
The so-called increase in death rate being propagated by strange unelected individuals with investments to protect involves absolutely negligible numbers - and that’s assuming even these numbers aren’t fabricated. WHO knows, at this point. Public distrust is at an all-time high due to the COVID-19 “mismanagement debacle”.
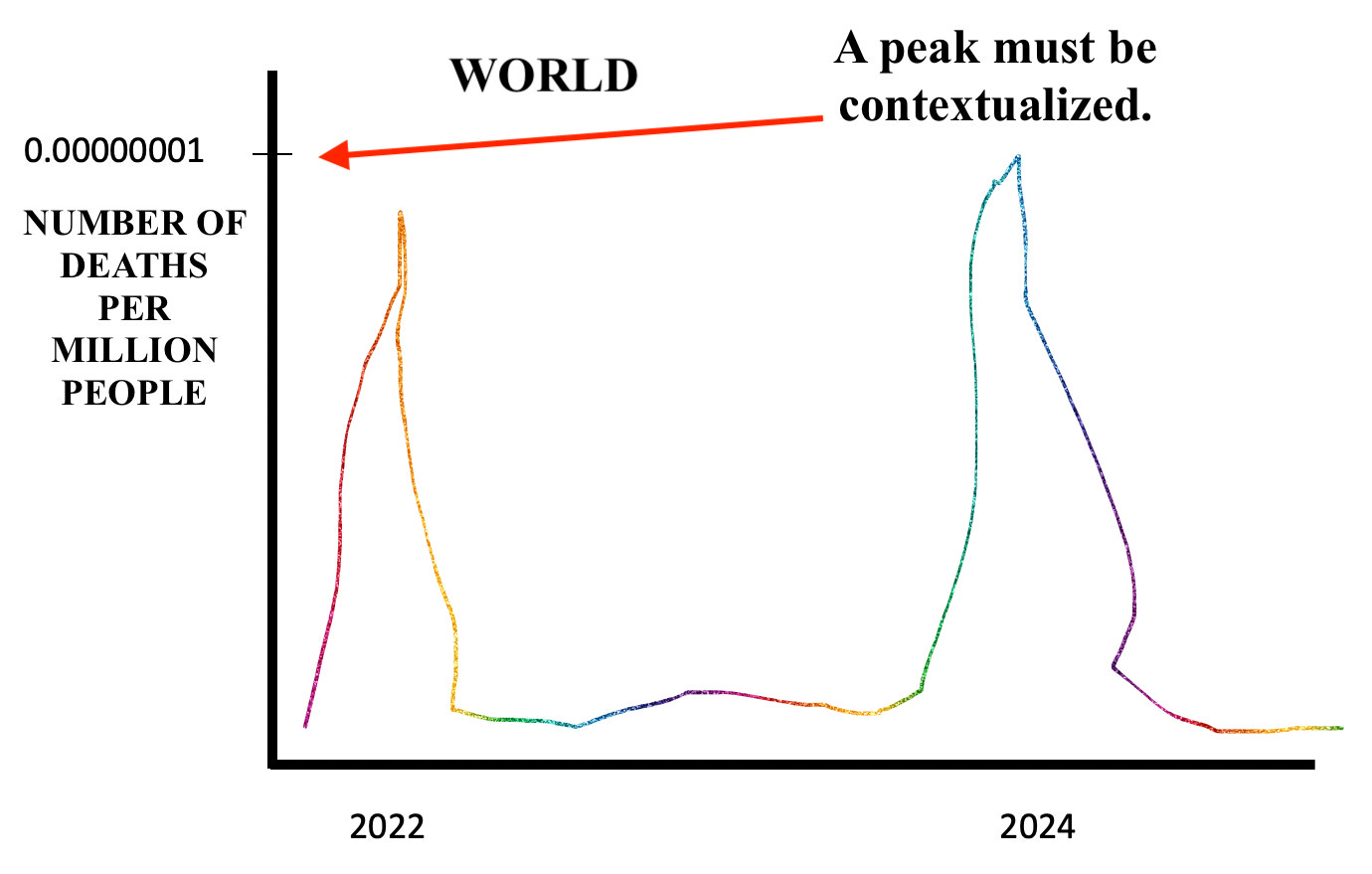
That so-called “peak” at the end of July (right before US election - cough, cough) represents - according to OWID - a rate of 0.0002 deaths per million people. That’s 0.0002/1,000,000 people.
That’s a 0.0000000002 chance, or a 1 in 5 billion chance of dying from mpox according to the current ‘case’ and ‘death’ rates. This does not a pandemic nor emergency make.
Let me demonstrate with an even better graph why these are simply really bad scare tactics.
From: Jessica Rose writing on Substack
By Peter A. McCullough, MD, MPH
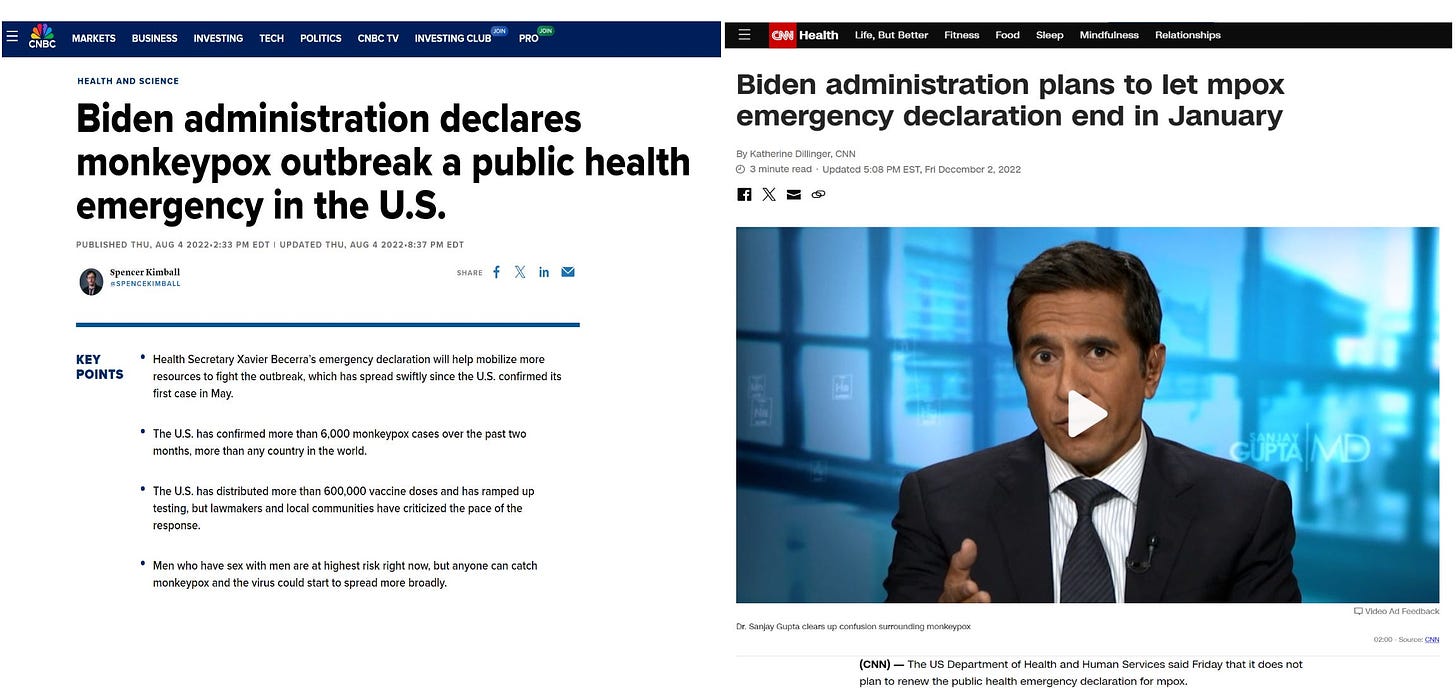
President Biden and HHS Secretary Becerra declared a US Monkeypox Public Health Emergency in 2022 and let the declaration expire early in 2023. The crisis conjured up little fear for the average American as it was learned that the infection was largely a pustular rash that occurred with intense sexual contact among gay/bisexual men with the skin blisters around the anus and buttocks or mouth. The CDC controlled PCR testing, the primary drug tecovirimat, and the Bavarian Nordic Jynneos vaccine. As of January 10, 2024, CDC stopped updating Monkeypox data because of low-level transmission of the clade 2 subtype in the U.S that resulted in 32,063 cases and 58 deaths largely among men with advanced HIV disease.
A report by Kannan et al, indicated that what happened in 2022 almost certainly occurred because of a gain-of-function mutation in one or more genes within the Monkeypox virus. The authors do not speculate on whether this happened in a laboratory or in nature.
Mutations in the monkeypox virus replication complex: Potential contributing factors to the 2022 outbreak
Journal of Autoimmunity Volume 133, December 2022, 102928
By Kannan et.al.
Abstract
Attributes contributing to the current monkeypox virus (MPXV) outbreak remain unknown. It has been established that mutations in viral proteins may alter phenotype and pathogenicity. To assess if mutations in the MPXV DNA replication complex (RC) contribute to the outbreak, we conducted a temporal analysis of available MPXV sequences to identify mutations, generated a DNA replication complex (RC) using structures of related viral and eukaryotic proteins, and structure prediction method AlphaFold. Ten mutations within the RC were identified and mapped onto the RC to infer role of mutations. Two mutations in F8L (RC catalytic subunit), and two in G9R (a processivity factor) were ∼100% prevalent in the 2022 sequences. F8L mutation L108F emerged in 2022, whereas W411L emerged in 2018, and persisted in 2022. L108 is topologically located to enhance DNA binding affinity of F8L. Therefore, mutation L108F can change the fidelity, sensitivity to nucleoside inhibitors, and processivity of F8L. Surface exposed W411L likely affects the binding of regulatory factor(s). G9R mutations S30L and D88 N in G9R emerged in 2022, and may impact the interaction of G9R with E4R (uracil DNA glycosylase). The remaining six mutations that appeared in 2001, reverted to the first (1965 Rotterdam) isolate. Two nucleoside inhibitors brincidofovir and cidofovir have been approved for MPXV treatment. Cidofovir resistance in vaccinia virus is achieved by A314T and A684V mutations. Both A314 and A684 are conserved in MPXV. Therefore, resistance to these drugs in MPXV may arise through similar mechanisms.
BigMouth comment: It seems highly unlikely that this constellation of mutations related to drug resistance and increased transmissibility happened in a pangolin or other wet-market fare in a very short period of time. Furthermore Dr. McCullough indicates that one of these mutations is a sign of gain-of-function genetic laboratory manipulation contributing to the current outbreak.
12-Year-Olds Could Get Mpox Vaccine in EU if Approved
Bavarian Nordic today said it plans to seek European regulatory approval for its mpox vaccine for children ages 12-17. Meanwhile, medical commentator John Campbell, Ph.D., today said he believes the probability of “ongoing sustained transmission” of mpox in the West is “remarkably low.”
It's begun: the effort to get novel vaccines into Africans
By Meryl Nass, writing on Substack
This information is from the Aug 13 and 14 briefings on monkeypox in Africa, mainly in the Democratic Republic of Congo. The next post will be a slide deck looking more closely into the claims.
Notes from Tedros’ press briefing on August 14:
WHO is working with the governments of the affected countries, the Africa CDC, NGOs, civil society and other partners to understand and address the drivers of these outbreaks.
WHO has developed a regional response plan, requiring an initial US$ 15 million to support surveillance, preparedness and response activities.
To fund that response we have released US$ 1.45 million from the WHO Contingency Fund for Emergencies, and we plan to release more in the coming days. We are also appealing to donors to fund the rest of the response plan.
As you know, two vaccines for mpox are recommended by WHO’s Strategic Advisory Group of Experts on Immunization, and are also approved by WHO-listed national regulatory authorities, as well as by individual countries including Nigeria and the DRC.
Last week I triggered the process for Emergency Use Listing for mpox vaccines, which will accelerate vaccine access for lower-income countries which have not yet issued their own national regulatory approval.
Emergency Use Listing also enables partners including Gavi and UNICEF to procure vaccines for distribution.
WHO is grateful to Member States and vaccine manufacturers for working with us on vaccine donations.
Africa public health body declares mpox emergency
August 14, 202410:36 AM EDT Updated 2 hours ago
Aug 13 (Reuters) - Africa's top public health body declared what it termed a "public health emergency of continental security" on Tuesday over an outbreak of mpox that has spread from the Democratic Republic of Congo to neighbouring countries.
[The former head of this agency is John Nkengasong, who now works for the US State Dept. as the lead on Global Health Security with title of Ambassador. The current head of the Africa CDC, Jean Kaseya has been investigated for corruption. It’s safe to say the agency does what its funders and string-pullers tell it to do.]
The Africa Centres for Disease Control and Prevention (Africa CDC) had warned last week of an alarming rate of spread of the viral infection, which is transmitted through close contact and causes flu-like symptoms and pus-filled lesions.
Most cases are mild but it can kill.
"We declare today this public health emergency of continental security to mobilize our institutions, our collective will, and our resources to act swiftly and decisively," Director General Jean Kaseya said in a briefing that was live-streamed on Zoom.
The outbreak in Congo began with the spread of an endemic strain, known as Clade I. But the new variant, known as Clade Ib, appears to spread more easily through routine close contact, particularly among children.
Kaseya said in the briefing that the continent needs more than 10 million doses of the vaccine, but only about 200,000 are available. He promised that Africa CDC would work to quickly increase the supply to the continent.
"We have a clear plan to secure more than 10 million doses in Africa, starting with 3 million doses in 2024," he added, without saying where the vaccines would be sourced.
The health body said that more than 15,000 mpox cases and 461 deaths were reported on the continent this year so far, representing a 160% increase from the same period last year. A total of 18 countries have reported cases.
Mpox has been endemic in parts of Africa for decades (or longer) after it was first detected in humans in the Democratic Republic of Congo in 1970.
A milder version of the virus spread to more than a hundred countries in 2022, largely through sexual contact, prompting the World Health Organization (WHO) to declare a public health emergency of international concern, its highest level of alert.
The WHO ended the emergency 10 months later, saying the health crisis had come under control.
The U.S. Centers for Disease Control and Prevention (CDC) issued a second health alert last week to notify clinicians and health departments about the deadly new strain.
Also last week, Africa CDC said it had been granted $10.4 million in emergency funding from the Africa Union for its mpox response.
WHO chief Tedros Adhanom Ghebreyesus has promised to convene an emergency committee to discuss whether the outbreak in Congo represents a public health emergency of international concern.
Reporting by Jessica Donati; Editing by Alex Richardson and David Holmes
The Africa CDC was established in 2017. Here are its goals, clearly aligned with the biosecurity agenda. Clearly the main African killers, Tuberculosis and Malaria, are not a big concern.
Objectives https://africacdc.org/about-us/
Establish early warning and response surveillance platforms to address all health threats and health emergencies and natural disasters in a timely and effective manner.
Assist Member States to address gaps in capabilities required for compliance with the International Health Regulations (IHR 2005).
Support and/or conduct regional- and country-level hazard mapping and risk assessments for Member States.
Support Member States in health emergency responses, particularly those which have been declared a public health emergency of international concern (PHEIC).
Support health promotion and disease prevention through health systems strengthening, by addressing infectious and non-communicable diseases, environmental health and NTDs.
Promote partnership and collaboration among Member States to address emerging and endemic diseases and public health emergencies.
Harmonize disease control and prevention policies and the surveillance systems in Member States.
Support Member States in public health capacity-building through medium- and long-term field epidemiological and laboratory training programmes.